The following is a quick overview of my past 7 weeks.
BEFORE SURGERY
Foods to buy might include: bananas, rice crackers, soups (chicken broth based soups and probably nothing cream based unless you enjoy crapping yourself or vomiting), ginger tea and whatever else your mom might whip up for you. My mom made me roasted tomato soup that I ate for a few days and seemed to warm my stomach. Stay away from carbs and anything that will take too long to digest. After about a week I made fruit smoothies and ate a lot of soup.
Items to have handy include: A large heating pad (I laid on a heating pad for weeks) and a large magic bag you can drape over your shoulders to assist with the incessant gas pain.
Days Off for Surgery: I did not think I would require any time off for recovery other than the day of the surgery. I was very wrong on that assumption. My surgery was on a Wednesday. I was in bed Thursday/Friday, very slow and weak Saturday/Sunday, and worked from home the entire next week. I would say you should plan for 5 days of complete down time unless you want to pass out from pain. If you end up needing less than 5 days - great! When I did work from home, I laid out on the couch with my laptop on my thighs because sitting up in a desk-like position really hurt my insides. I would say 2 weeks is a healthy estimate until you're feeling semi-normal again.
AFTER SURGERY
Days 1-5: I was taking pain pills every 3-4 hours. I alternated between tramadol and naproxen (both prescribed after surgery) and T3's and Advil (from my ongoing pain regime) for the first week. I went back to the doctor on day 5 and got more Tramadol. I went to the doctor again 2 weeks after for antibiotics (see below). I bled slightly for the first 3 days. My lower back was extremely sore to the point where I would almost vomit after my daily walk. I tried to walk about 5km, very slowly, every day, to try and shift the gas around my innards. The gas pain had lessened by day 5, however days 1-3 were still very very painful. It is hard to put words to the gas pain but it is the worst inescapable pain I have experienced to date. You'll get through it, but while you're writhing in pain and unable to find a comfortable position to sleep in, know that we have all experienced a similar hell (and you are most welcome to commiserate if you feel the same upon reading this).
Day 6: I was able to poop for the first time. This was after several days of drinking restorolax, drinking coconut oil, taking ex-lax chocolates and eventually resorting to a glycerine suppository because the discomfort got too much for me to handle.
Day 7: I was able to finally sleep on my side and the gurgle, air-filled belly feeling was mostly gone. The first week I was sleeping on my back with a big pillow folded under my knees. Doing any kind of a sit up or belly-tightening was impossible and painful. I would roll sideways like a whale, and slide out of bed upon waking up. It was a highly attractive little maneuver. I was sleeping and resting on my heating pad any time I was laying down on the couch or in bed.
Day 8: My appetite came back. The first 8 days I did not feel like eating and I ended up losing a bunch of weight (don't worry -- I have eaten it all back on now).
My belly button incision was infected and not healing about 2 weeks after surgery. I took 7 days of 4x a day antibiotics and applied a topical cream. It took about 5 weeks before my incision healed and it is still sore today, 7 weeks later. It healed a little messed up and I have since decided to leave my belly button ring out.
Activities: I had to travel for work 2 weeks after the surgery date and it was honestly too much (the pain and my random outbursts of tears made for a hellish 4 day trip). Try not to plan anything too crazy for the first few weeks -- you'll thank yourself. Treat your body kindly - when you can't see the damage you don't end up treating your body as nicely as you would if your entire abdomen and pelvis were burnt and bleeding everywhere for the world to see!
Listen to your body. If you feel sore or slow: rest. If you are in pain that is not lessening: see your doctor or go to emerg. If you take way longer to heal than most of the stories you have read, don't be upset: be kind to your body. It is a lot to ask of a body to be in pain for years on end, to be surgically excised and to continue working like normal. We are warriors, but also need to give ourselves some time to rest and recover, however long that may be.
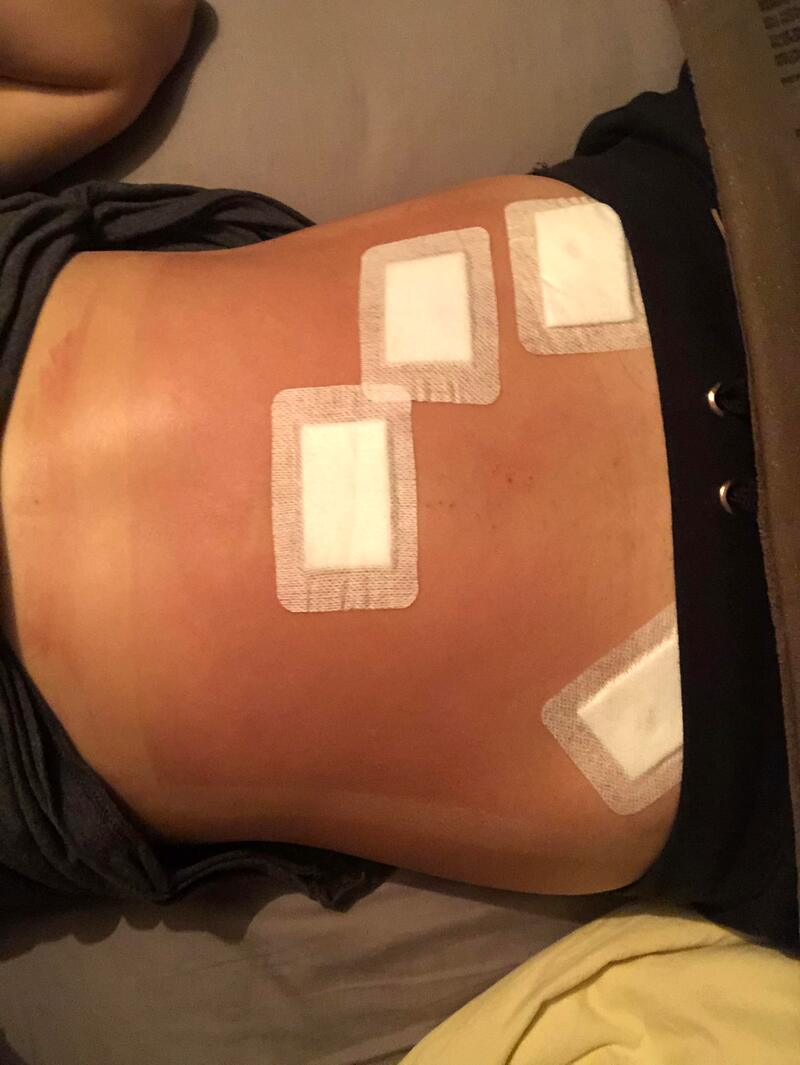
SCARS
EMOTIONS
I felt humbled and thankful to live in Canada and to have received top of the line medical care from an endo specialist in my own city. I am so very cognizant that there are women who will fight the pain and various other symptoms of this disease for their entire lives with no help from the medical system (for whatever reason that may prevent treatment). I know that this experience has made me vow to be more vocal and to make sure that endometriosis is a word in everyone's vocabulary. It is stifling the number of people who have no idea what endo is and I have made it my mission to educate and spread awareness -- one person at a time.
6 WEEK FOLLOW-UP APPOINTMENT
I have also been thinking a lot about the genetic links between women in a family -- I would be interested in hearing from anyone who has had suspected endo present over generations of women in their families. I am trying to draw my own conclusions but only have my personal experience to speak to.































































































 RSS Feed
RSS Feed
